* ‘CHANGING A CULTURE’ WITHIN THE BOP. * IMPLEMENTING THESE CHANGES – SOUNDS EASY. WHAT IF NO ONE’S LISTENING? * THE FULL BENEFIT OF THE FSA AND SCA IS TRIGGERED WITH SENTENCES OF OVER 74 MONTHS * (UNDER AND OVER 60 MONTHS,
Read More
PANIC – ANGER – “THIS CAN’T BE HAPPENING” * HOW DO YOU COUNTER THE INITIAL FEAR AND PANIC OF THE UNKNOWN? * Find a Group or Someone To Talk To Someone Who’s Been Through This – You’re Not Alone * ⇓ This
Read More
HOW DO YOU COUNTER THE FEAR OF THE UNKNOWN? WHAT CAN YOU DO? S Find a Group or Someone To Talk To Someone Who’s Been Through This – You’re Not Alone ⇓ This White-Collar Support Group is a Great First Start ⇓
Read More
* WHITE-COLLAR PROVIDER SPECIALISTS – TELEHEALTH – PHARMA. * WHILE THE CHARGES MAY START CIVIL (FINANCIAL), TAKE THESE SERIOUSLY. CIVIL TODAY CAN BECOME CRIMINAL TOMORROW. FIRST, GET LEGAL ADVICE. A A SHOULD YOUR CHARGES BECOME CRIMINAL WHETHER BY PLEA OR TRIAL, CONSIDER
Read More
* THEIR FIRST TARGET IS YOU: WHITE-COLLAR HEALTHCARE, AND LIFE SCIENCES. * WHILE THE CHARGES TODAY ARE CIVIL AND FINANCIAL, TAKE THESE SERIOUSLY. CIVIL TODAY CAN BECOME CRIMINAL TOMORROW. FIRST, GET LEGAL ADVICE. A A SHOULD YOUR CHARGES BECOME CRIMINAL… WHETHER
Read More
HOME CONFINEMENT THIS 6/17/2025 PRESS RELEASE APPEARS TO HAVE SOME TEETH BEHIND IT ONLY TIME WILL TELL * GETTING INTO THE DETAILS OF THE SECOND CHANCE ACT If your sentence is > 60 mo (5 yrs) = last 6 mo on home confinement.
Read More
** PRIORITIZING INDIVIDUALS WHO DO NOT NEED STRUCTURED SUPPORT – TO HC. 6/17/2025 FSA [First Step Act] and SCA [Second Chance Act], cumulatively applied in sequence to maximize prerelease custody. Residential Reentry Center (RRC) Bed Availability/Capacity Shall Not Be a Barrier to
Read More
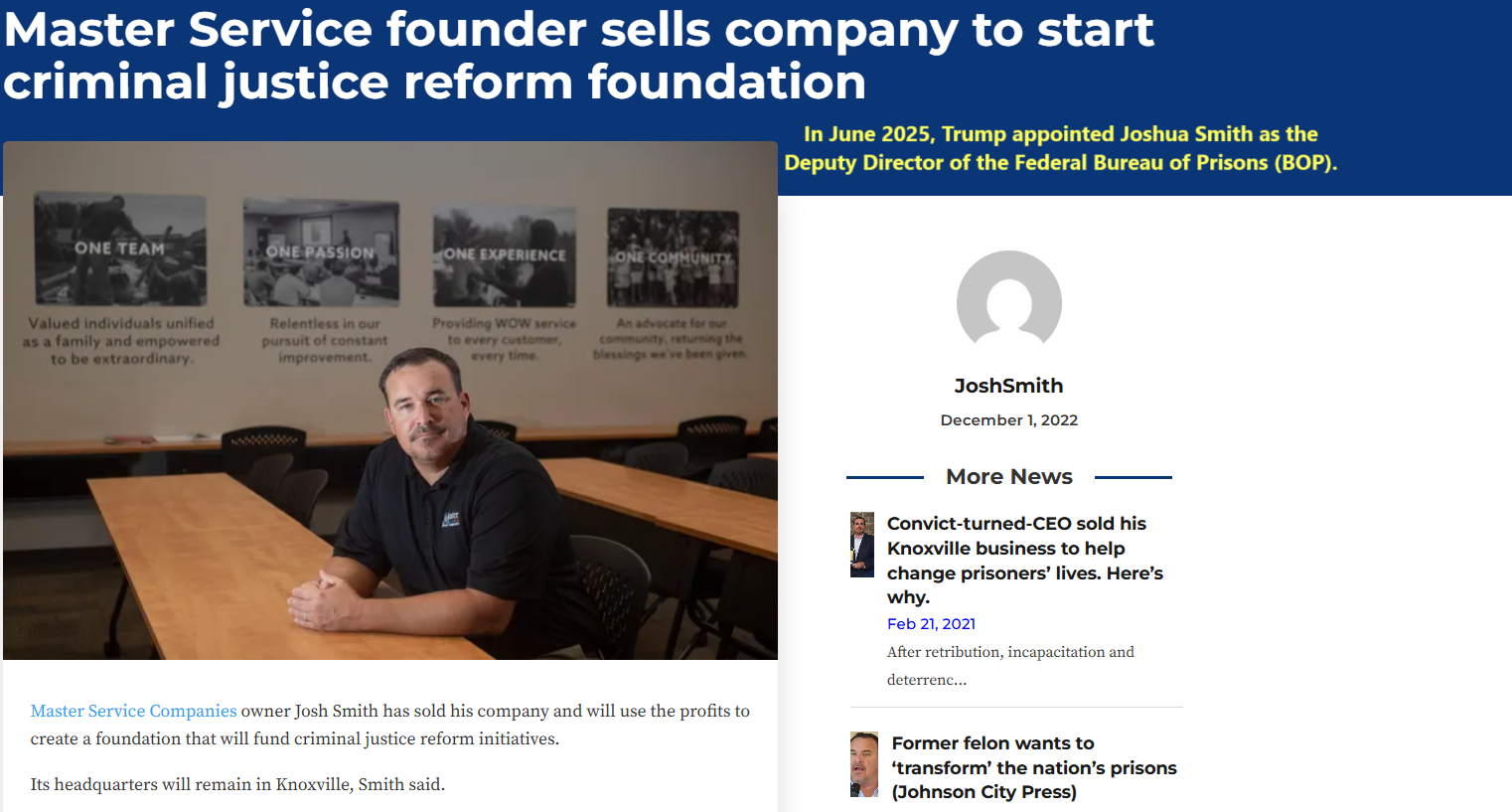
Who is Joshua Smith – the next Deputy Director of the Federal Bureau of Prisons? Joshua Smith spent five years behind bars in Kentucky for his involvement in drug trafficking, then in 2025, Smith was awarded a full pardon Wednesday by President
Read More
False Claims Act (FCA), Coding – falls into: “fraud (intentional)” or “abuse (innocent mistake).” * The #1 Target that the DOJ Criminal Division will prioritize and investigate begins with Healthcare and Procurement Fraud—memorandum: May 12, 2025. A What was once considered criminal,
Read More
His Defense Team (Agnifilo Intrater LLP), Led By Teny Geragos, is one of the Best. NOTHING IS GUARANTEED. DIDDY COMBS HAS A ‘GREAT LEGAL TEAM,’ AND SHOULD FOLLOW THEIR RECOMMENDATIONS. We hope he will heed their advice. * * * 6/1/2025. Trump Responds
Read More